A cancer diagnosis is never good news, but one for pancreatic cancer is among the most challenging. With five-year survival rates for patients as low as 3-15%, it is the most lethal of the common cancers in the UK and globally. To make matters worse, 8 in 10 patients cannot even be offered potentially life-saving surgery because the cancer is too advanced when first detected.
The problem is compounded because, unlike breast cancer for example, it’s hard for people to detect their own cancer, and there’s no regular screening because there are currently no established biomarkers for early signs of the condition.
Improving early detection times is therefore the primary goal to improve patient outcomes. UK-EDI is headed up by Professor Eithne Costello, a molecular biologist based at the University of Liverpool’s Department of Molecular and Clinical Cancer Medicine, who with colleagues is working on the development of novel approaches to detect pancreatic cancer early in people newly diagnosed with type 2 diabetes.
The connection with diabetes is that at the time of cancer diagnosis, well over half of all pancreatic cancer patients have elevated blood sugars with 3 in 10 having recently become diabetic. The diabetes precedes the cancer by a year or so, and this window is when a timely intervention can save lives.
UK-EDI is recruiting 2,500 people aged 50 years or older who have been diagnosed with diabetes within the last six months. Blood samples and clinical data will be collected from participants at appointments every six months for two years. Comparisons between those that do and those that do not go on to develop pancreatic cancer should help researchers pinpoint biomarkers for this deadly disease.
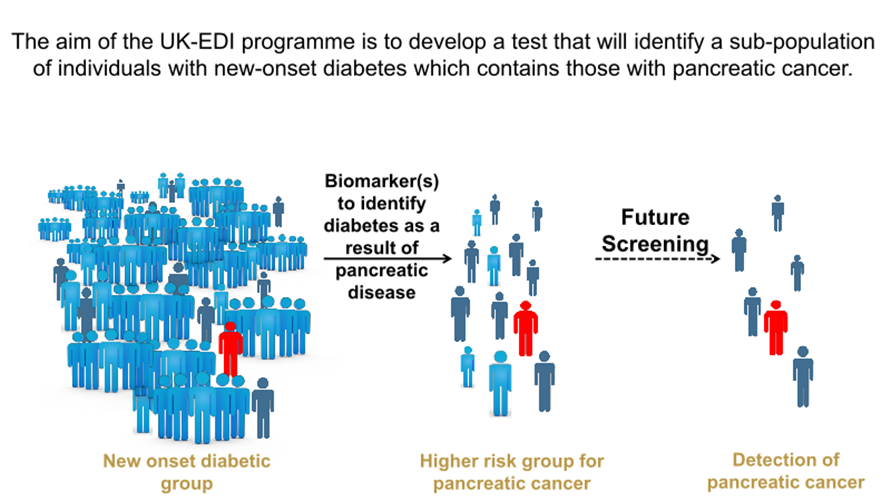
It should be borne in mind however that the majority of people who develop type 2 diabetes will not go on to develop pancreatic cancer. Approximately only 1 in 100 people with new-onset diabetes will subsequently be diagnosed with pancreatic cancer. For this small group of individuals the diagnosis of diabetes is believed to be an early sign of pancreatic cancer rather than the cause of the cancer. It is hoped that the samples as well as the clinical information collected from these participants will provide vital clues about biological events occurring before pancreatic cancer is diagnosed, allowing it to be detected earlier in future.
The promise of the diabetes connection means other research groups are also on the same track. UK-EDI collaborates with international colleagues; the Consortium of Chronic Pancreatitis, Diabetes and Pancreatic Cancer in the US and EUPancreas– a European research network, in order to improve the outlook for this most challenging condition.
UK-EDI has been developed with the involvement of the Liverpool Pancreatic Patient Advisory Group to ensure that our research meets the needs of the patients.
For more information about pancreatic cancer please follow this link and to find out about associated research into the early detection of pancreatic cancer click here
See the below video for a presentation on UK-EDI that was given at the June 2020 European Pancreatic club meeting